Biography
With expertise in neuroimmune biology and inflammation, Dr Barry McColl’s work aims to identify new treatment targets in this exciting field. Obtaining his PhD in Neuroscience from the University of Glasgow in 2004, he went on to complete postdoctoral training at the University of Manchester, joining The Roslin Institute at the University of Edinburgh in 2010 as a Tenure-track Fellow. He joined the UK DRI at Edinburgh in 2017 to lead a novel programme of research investigating how microglia influence resilience and susceptibility to neurodegenerative and vascular diseases that are causes of dementia.
News
Key publications
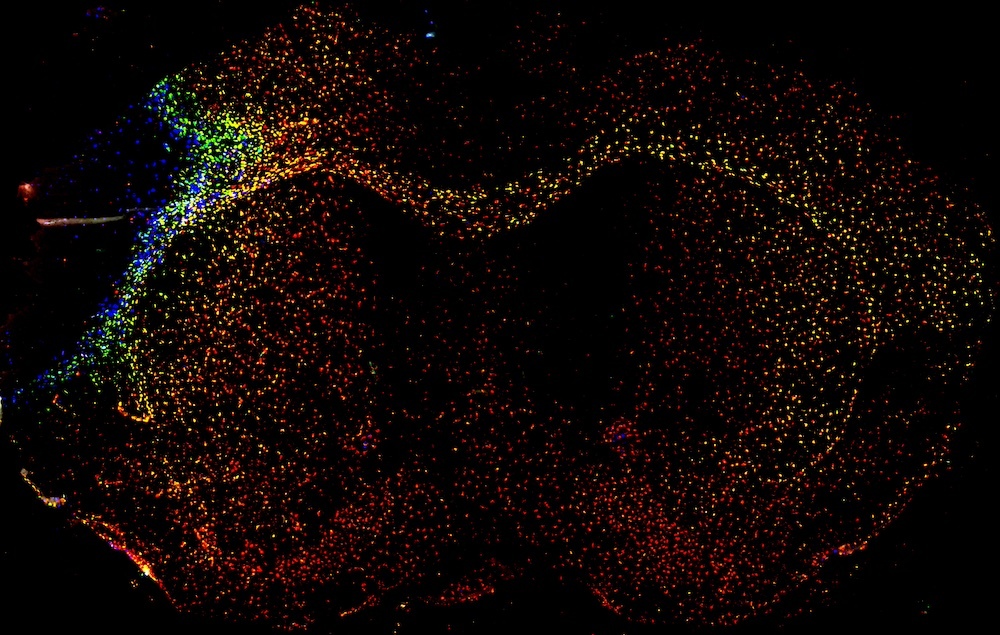
McColl Lab
Explore the work of the McColl Lab, Investigating the role of microglia in neurodegenerative disease