Key details
Transforming dementia diagnosis
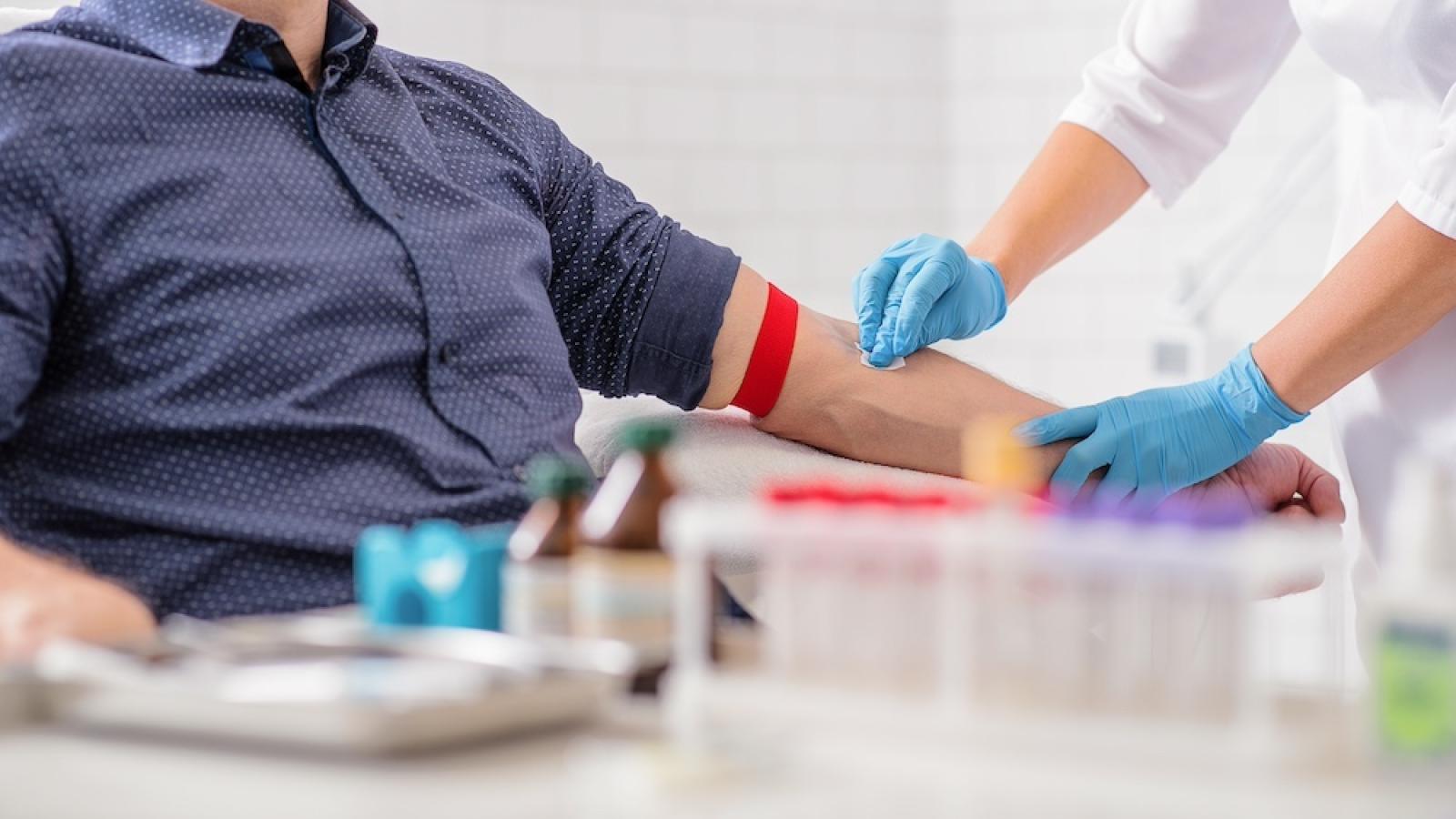
Dementia is one of the leading health challenges of ageing societies, with Alzheimer’s disease as the most common cause. Genetics and life experiences shape risk and resilience, but current diagnosis often comes too late for effective treatment. Early, accurate identification of dementia subtypes is vital for delivering appropriate care, enabling access to new therapies, and designing prevention strategies.
The Schott Lab addresses this by integrating data from long-term population cohorts with advanced biomarkers, including blood tests, spinal fluid, brain imaging, genetics, sleep and movement tracking, and digital cognitive assessments. The team has pioneered studies in the British birth cohorts, identifying life-course influences on brain health and validating blood-based markers such as plasma p-tau217 for detecting preclinical Alzheimer’s. They are also testing digital tools like remote cognitive and sleep monitoring to spot early changes at scale.
This work could transform dementia care by enabling inexpensive, widely available diagnostics, allowing population-level screening, earlier interventions, and more efficient trials of disease-modifying treatments—ultimately helping delay or prevent the onset of dementia symptoms
Latest news

Prof Jonathan Schott
Prof Jonathan Schott is a Group Leader at the UK DRI at UCL. Find out more about his career and expertise on his profile page.

Research summary
CEREBRAL: Cohort-based Epidemiological Research Employing Biomarkers to Reveal Alzheimer’s in Later life
Dementia, particularly Alzheimer’s disease (AD), represents one of the most pressing societal challenges of our time, with ageing the greatest risk factor. Epidemiological and genetic studies demonstrate that life-course exposures – cognition, education, socioeconomic status, vascular health, and lifestyle – shape risk and resilience. However, current diagnostic paradigms identify disease only after symptoms emerge, missing the long preclinical window where interventions may be most effective. Novel blood-based biomarkers, digital phenotyping, and multimodal imaging now provide the opportunity to transform early diagnosis, stratify risk, and accelerate trials of disease-modifying therapies.
In work completed to date the Schott Lab has integrated deep phenotyping of the 1946 British Birth Cohort (Insight 46) with multimodal biomarkers (amyloid and tau PET, MRI, CSF/blood assays, proteomics, genetics, cognition, sleep, movement). They demonstrated that plasma p-tau217 predicts PET evidence of AD pathology years in advance, identified life-course factors shaping risk trajectories, and established digital cognitive and sleep measures as scalable functional markers. These advances underpin translation of fluid biomarkers (notably plasma p-tau217) into NHS diagnostic pathways and have already informed policy and clinical trials.
This programme, CEREBRAL, builds on this foundation, extending longitudinal analyses across successive British birth cohorts (1946, 1958, 1970), incorporating novel biomarker platforms (e.g. NULISA proteomics, finger-prick plasma assays), advanced computational modelling, and remote digital assessments. This approach will deliver insights into life-course determinants of dementia, validate scalable diagnostic tools, and explore optimal means of predicting clinical progression.
Programme objectives
- Identify life-course determinants of dementia risk and resilience by integrating biomarker, genetic, and epidemiological data from UK population cohorts.
- Optimise early, scalable detection of preclinical Alzheimer’s disease through validation of plasma p-tau217 and multiplexed biomarker panels, including finger-prick testing.
- Develop and validate remote digital tools (cognitive and sleep measures) as functional markers of presymptomatic disease for use in trials and population screening.
- Apply advanced computational models to integrate multimodal datasets, quantify disease heterogeneity, and improve trial design and prognostication.
Key publications
Vacancies
Lab members
Collaborators













Lab funders
Thank you to all those who support the Schott Lab!